COVID’s health spillovers
Interesting paper from Ziedan, Simon and Wing (2023):
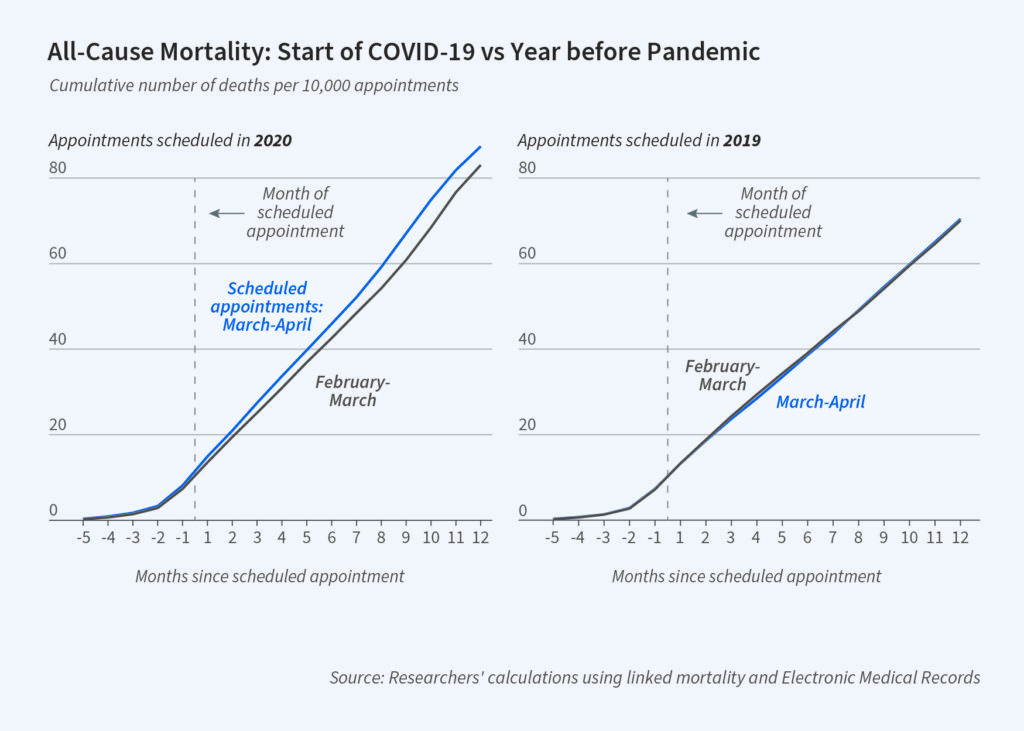
The contraction in health care consumption at the start of the pandemic provides insight into central economic questions of waste and productivity in the U.S. health care system. Using linked mortality and Electronic Medical Records, we compare people who had outpatient appointments scheduled for dates in 30 day periods immediately before and after the Covid-19 emergency declaration. Appointment cancellation rates were 77% higher for people with appointments in the shutdown period. Intent to treat estimates imply that having a scheduled appointment date right after the emergency declaration increased one-year mortality rates by 4 deaths per 10,000. Instrumental variable estimates suggest that a cancelled appointment increased one-year mortality by 29.7 deaths per 10,000 among compliers, implying that a 10% increase in health care appointments reduces mortality rates by 2.9%. The mortality effects are rooted in two mechanisms: a complier sub-population with high marginal benefits from care, and a cascade of delayed or missed follow-up care that lasted for about 3 months. Healthcare spending accounted for 19.7% of U.S. GDP in 2021, and controlling health spending is a major policy objective. Our results quantify health tradeoffs from cutting every-day non-emergency visits, illustrating the importance of cost-control efforts that differentiate between medical care with the largest and smallest benefits for patient health.
https://www.nber.org/bh/20231/costs-and-consequences-covids-impact-non-urgent-care
Also in the NBER Bulletin on Health, Acton et al. (2022) find that:
…college vaccine mandates reduced new COVID-19 cases by 339 per 100,000 county residents and new deaths by 5.4 per 100,000 residents, with an estimated value of lives saved between $9.7 million and $27.4 million per 100,000 residents. These figures suggest that the mandates reduced total US COVID-19 deaths in autumn 2021 by approximately 5%.
The full NBER Bulletin on Health is here.







