Why don’t physicians accept Medicaid patients?
One reason is that reimbursement rates for Medicaid are lower than for Medicare or commercial insurance. Another (often overlooked) factor, however, is physician’s risk of payment denials and the administrative hassle they face trying to get reimbursed by Medicaid. A paper by Dunn et al. (2024)–cleverly named “A Denial a Day Keeps the Doctor Away“–shows that reimbursement denials by Medicaid are much higher than for Medicare or commercial insurance.
Who bears the consequences of administrative problems in health care? We use data on repeated interactions between a large sample of U.S. physicians and many different insurers to document the complexity of health care billing, and estimate its economic costs for doctors and consequences for patients. Observing the back-and-forth sequences of claim denials and resubmissions for past visits, we can estimate physicians’ costs of haggling with insurers to collect payments. Combining these costs with the revenue never collected, we estimate that physicians lose 18% of Medicaid revenue to billing problems, compared with 4.7% for Medicare and 2.4% for commercial insurers. Identifying off of physician movers and practices that span state boundaries, we find that physicians respond to billing problems by refusing to accept Medicaid patients in states with more severe billing hurdles. These hurdles are quantitatively just as important as payment rates for explaining variation in physicians’ willingness to treat Medicaid patients. We conclude that administrative frictions have first-order costs for doctors, patients, and equality of access to health care. We quantify the potential economic gains—in terms of reduced public spending or increased access to physicians—if these frictions could be reduced and find them to be sizable.
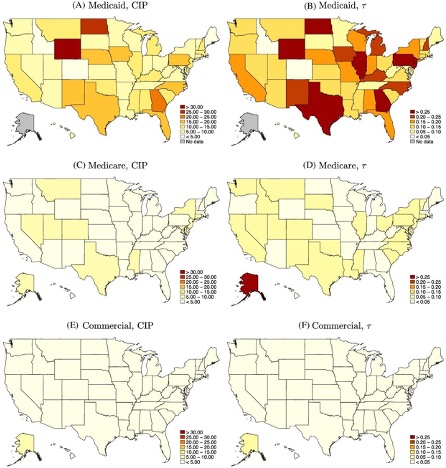
“The left column shows the mean estimated costs of incomplete payments (CIP) by state and payer.
The right column shows the mean CIP as a share of visit value by state and payer.“
Economist Writing Every Day has a nice summary of the issue.







